I am an independent Data Scientist with a PhD in Mathematical Psychology seeking data and collaboration for analyzing the relationship between early childhood trauma and adult mental disorders. My theoretical perspective on this work is that the current semantics describing mental disorders is too ambiguous to support a sustainable and effective Mental Health System. My approach to this problem is to relate the huge body of Experimental Psychology data to Mental Health data using a Human Information Processing Framework to characterize mental disorders. The components of this framework are attention (processor), memory (storage), sensing (raw impression), perception (labeling) and the cognitive strategies (software) that link these capabilities into a goal directed behavior. Mental disorders will be characterized in terms of mismatches between cognitive strategies and the information processing demands of a disorder-triggering situation. For example, can we predict adult bias to switch attention to the right brain (“dissociate”) during stress when that adult experienced trauma before age three (primarily right brain processing)?
Interesting.
The only problem that we mostly work with a clinical data level: diagnoses, procedures, lab tests standardized inventories and questionairies (when it comes to the assessment of mental health), so we never see the details you described.
First, we might run some characterization study trying to find patients with documented abuse or neglect in childhood, and see the prevalence of mental disorders in their adulthood. Might be pretty interesting if you include the socio-economic, race, country etc in the characterization.
If psychopathology is reduced to a list of commonsensically derived and simplified
operational features, further progress of pathogenetic research will be seriously
impeded. What is needed is a complex psychopathology capable of mediating between
symptom level and process level, and of developing models of the inherent structure
and possible disturbances of conscious experience.
(Fuchs 2010, p. 269)
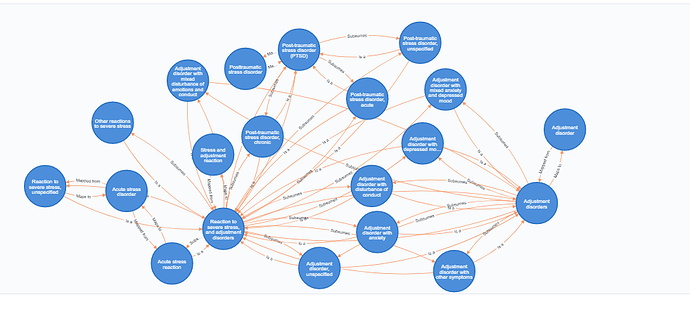
Seeking funding for mapping mental illness phenomenology to standard ontologies
Disabilities related to mental health are among the overall fastest growing threats to global health with depression being the leading threat. However, science is failing to keep up with the challenge because the vocabularies being used to label the patient’s experience are not standardized leading to an obvious “garbage in, garbage out” situation for any analytics performed on those mislabeled pieces of data. My research aim is to develop a semantics framework that relates patient descriptions of their experiences to standard ontologies that connect these experiences to the biology, neurology, neuropsychology, psychology and psychiatry ontologies. This mapping will provide a common language for all disciplines studying factors related to mental health to share and collaborate on finding relief for people suffering from these experiences.